What’s the Deal With Temperature Checks? 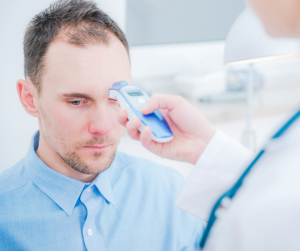
As businesses start re-opening, we will come into contact with more people and the microbes they carry with them. Airlines, gyms, hair salons and restaurants are examples of places where an additional layer of protection can go a long way to help our economy remain open and avoid a ‘second wave’ of COVID-19.
SDSM has been implementing safe social distancing and interactions for many weeks now by asking every patient about recent fever, cough, cold or flu symptoms, recent travel, contact with anyone experiencing any of the above, and taking temperatures of those entering our facilities. Without the success of social distancing measures, San Diego would not now be enjoying the lifting of stay at home measures. Early detection and prevention will continue to be paramount for some time and taking temperatures is just one way to identify early illness. You will see many businesses using this practice to keep employees and patrons safe.
Why are temperatures useful?
Viral illnesses can seem to appear out of nowhere with the first sign being that of an elevated temperature. The immune system uses an increase in body temperature to help fight a virus that has entered the body. By the time you feel that you have a fever, the virus has had the potential to be spread far and wide. Catching the initial rise in body temperature, before you feel it, may provide precious time necessary to isolate an infectious person and contain an infection. As we know, isolation of an active infection prevents its spread.
Recent studies on COVID-19 have reported fever as a symptom but it seems to vary with the progression of the disease. In New York, 31% of patients had a fever >100.4 F at the time the patient presented for care. In Wuhan and other areas in China, axillary temperatures over 99.5 F where found in 44% of patients on admission. Studies on hospitalized patients have indicated a fever in 89-99% of cases. These temperature discrepancies are why we should not rely on body temperature alone as an early indicator of disease. Other symptoms to evaluate include loss of taste or smell, nausea, diarrhea, headache, sore throat, and runny nose. These are typical of many viral infections.
What is normal?
A normal oral temperature is considered to be 98.6 F. A person is said to have a fever with a core temperature of 100.4 F. There are natural body temperature fluctuations that are no cause for concern. Core temperatures are usually lower in the morning, a bit higher during the day, and may lower again at night. Hormonal cycles influence body temperature fluctuations, as does exercise, overexertion, or exposure to heat such as sitting in a sauna or jacuzzi. Human temperature might also be evolving, as found in this recent study from Stanford University. On average, humans have lost a degree of body temperature since the 1800’s. Environmental changes leading to overall better health, less inflammation from communicable disease, and modern heating and cooling systems are thought to be influencing this trend.
NORMAL TEMPERATURES BY METHOD:
- Oral 98.6 F
- Rectal 0.5-1.0 degree higher than oral
- Ear (tympanic) 0.5 – 1.0 degree higher than oral
- Armpit (axillary) 0.5-1.0 degree lower than oral
- Forehead (temporal) 0.5-1.0 degree lower than oral
How do you take a temperature?<
Knowing how to take a temperature and using an accurate measuring device is imperative. While rectal temperatures are the most accurate, thankfully they are unacceptable outside the medical facility! Oral temperatures are the next most accurate with ear, axillary (armpit), and forehead temperatures following in that order. An oral or armpit temperature will register 0.5-1.0 degrees lower than a rectal temperature, so add a degree to these results for the most accuracy.
We recommend safely disposing any mercury containing thermometers you may have and replace them with digital thermometers that can be used orally or in the armpit, or a rectal thermometer for babies and young children. Mercury is dangerous to humans and animals, is difficult to clean up safely, and will evaporate into the air exposing you, your family, and pets.
Here’s how to take an oral temperature:
- Wash hands thoroughly before touching the digital thermometer.
- Be sure you’ve had nothing to eat or drink for at least 5 minutes.
- Place the thermometer tip under the tongue in the same spot for 40 seconds or until the thermometer beeps or flashes complete.
- Remove the thermometer and record the temperature and time.
- Clean the thermometer with soap and water. You may also want to rinse it with alcohol, then rinse with water before storing.
Use of forehead scanners and ear thermometers vary so follow the manufacturers guidance or refer to these recommendations from the Cleveland Clinic.
What should employees and employers know?
The State of California has set re-opening guidelines for employers and businesses. It is in our best interests to adhere to these guidelines to prevent a second wave of COVID-19.
Employees:
- Check your temperature each day before going to work. This can prevent infecting other employees, prevent loss of income to employees and employers, and keep the business open.
- Report any flu like symptoms or elevation in temperature that is 99.5 F or above to your employer.
- Stay home if you have any flu like symptoms or fever and call SDSM for guidance on treating your symptoms and testing for COVID-19.
Employers:
Taking temperatures is considered handling of protected information so consult your local guidelines for your full responsibilities on handling this information. Guidelines vary by state and country. At the minimum:
- Determine who to test: employees, vendors, patrons.
- Determine the temperature cut-off for your workplace.
- 99.5 F will allow for the 0.5-1.0 degree lower result in oral or armpit temperatures that might not reflect a true core temperature.
- 100.0 F or 100.4. F are considered fevers by any method of temperature assessment.
- Determine the policy for those who refuse temperature assessment.
- Use a touchless thermometer like a forehead scanner, if possible.
- Take temperatures close to the entrance and practice all social distancing measures for those waiting to be scanned.
I have a fever, now what?
Take good care of yourself. COVID-19 or not, it’s good practice to isolate from others when you are ill. Fever and pain reducers can be taken if needed, drink plenty of fluids, and rest. Rest is the biggest help to the immune system which is most active when the body is allowed to rest. A fever of 103 F, or symptoms including chest pain, shortness of breath, severe head or neck ache may require medical attention.
Keep up the good work San Diego! Practice good social distancing measures, carry a mask and wear it when you risk coming within six feet of others, wash hands frequently, and take your temperature when appropriate. As always, SDSM is here for you to answer any questions or concerns you have about this or any other aspect of your health. Don’t hesitate to call!
Vitamin D: Not Just For Bone Health
Vitamin D is a top performer when it comes to health. We most often hear about Vitamin D and how it is essential for calcium absorption for maintaining healthy bones. But did you know that Vitamin D is important for proper mood regulation, immune function, cognitive function, and possibly protection from some cancers and Multiple Sclerosis?
Most of us do not get enough Vitamin D in our diet without careful planning or supplementation. Vitamin D works with Omega 3 fatty acids to facilitate calcium absorption in the intestines. It also regulates cell growth and differentiation which is important in maintaining bone mass and controlling the growth of new cells in the body. Vitamin D has also been tied to muscular strength. Both senior citizens and Olympic athletes experience improvements in muscle strength with improved Vitamin D status.
There is strong evidence that Vitamin D levels are associated with depression and anxiety. Vitamin D has characteristics of both a vitamin and a hormone and has been found to improve serotonin levels. It does this by regulating the gene that encodes for activation of tryptophan. Tryptophan is an essential amino acid for the formation of serotonin, one of the hormones responsible for feelings of well-being and happiness. Seasonal Affective Disorder may be improved by the addition of Vitamin D. Vitamin D levels naturally fluctuate during the year with levels rising in the summer during longer days with more sunlight, to lower levels in the winter. Individuals with low normal levels of Vitamin D in the summer can fall into inadequate or deficient levels during the winter. Vitamin D also seems to improve the body’s ability to control cancer growth including non-melanoma skin cancer. A 50% reduction of risk of breast cancer was observed in women with blood levels of 52 ng/ml, and a 50% reduction in colon cancer observed with blood levels of 34 ng/ml.
Vitamin D has gained recent attention in COVID-19 patients. Those with the worst symptoms have been found to have the lowest Vitamin D status. The role of Vitamin D in immune function has been well established, especially in the prevention of upper respiratory infections. Experts are considering poor Vitamin D status as a risk factor for COVID-19 and advising that Vitamin D status be addressed as a mode of prevention.
There is argument regarding how much Vitamin D each of us should consume each day. The NIH reports that 94% of 51-70 year olds fall well below an intake 600 IU per day, the amount necessary to prevent disease in most people. The best advice is to consider your individual lab results, health conditions, and even your complexion. The amount of melanin or pigment in your skin, affects the amount of Vitamin D your body can activate. More melanin means less Vitamin D is converted to the active form. This puts people of color at higher risk of Vitamin D deficiency. The active form of the vitamin is made by exposing 7-dehydrocholesterol in the skin to ultra violet B (UVB) light to make previtamin D. Previtamin D is then converted by the kidneys to the active form Vitamin D3. Although we derive active Vitamin D from sun exposure, it is not advised to attempt to maintain adequate Vitamin D levels through sun exposure. UV rays promote skin cancer, a topic we discussed in our May 8 newsletter.
Normal levels of Vitamin D range from 30-100 mg/ml. Normal levels differ from what may be considered optimal levels which the Institute of Medicine believes to be closer to 50 ng/ml, or the middle of the normal range. Those with compromised immune function, osteoporosis, Vitamin D deficiency, mood disorders, and people of color can benefit from individualized Vitamin D supplementation to optimize blood levels. Few foods contain high levels of Vitamin D in nature. Organ meats and mushrooms are amongst the highest in Vitamin D, with the former not well accepted nor appropriate for all to consume. Fortified dairy products and nut milks are the most commonly consumed food sources of Vitamin D, and it is also found in fatty fish like salmon, trout, and mackerel.
There are many reasons to optimize Vitamin D levels including protecting bone health and muscle strength, optimizing moods, and immune function. We recommend working with your provider or a Registered Dietitian to find the foods right for you and to learn how to include supplements if necessary.
Multi-system Inflammatory Syndrome in Children (MIS-C)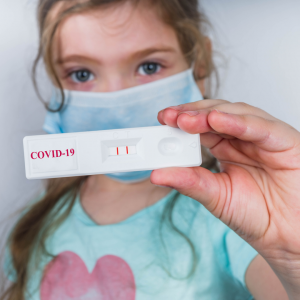
by Dr. Shannon Cheffet
After nearly three months of quarantine all of our heads are spinning about how and what we need to do to protect ourselves and our loved ones from this novel coronavirus. For months, we have heard that this virus predominantly affects those over 65 years of life and those with “co-morbid” medical conditions. However, in the last few weeks, parents are likely feeling rising concern about the reports of a rare, but potentially severe, inflammatory response to COVID-19 in children. The CDC and World Health Organization are closely monitoring reports of approximately 200 children under the age of 18 who presented with severe inflammatory symptoms involving more than one body system. Once a possible link of this inflammatory condition was linked with COVID-19, the CDC compiled a list of concerning symptoms to help guide parents.
Symptoms that warrant contacting your child’s doctor are:
- Fever
- Abdominal pain
- Vomiting
- Diarrhea
- Neck pain
- Rash
- Bloodshot eyes
- Feeling extra tired
Symptoms that warrant emergency room evaluation would be:
- Trouble breathing
- Pain or pressure in the chest that does not go away
- New confusion
- Inability to wake or stay awake
- Bluish lips or face
- Severe abdominal pain
The presentation of the this new MIS-C condition mirrors in many ways a well known inflammatory condition for children, called Kawasaki Disease. Some of the clinical criteria to diagnose Kawasaki is fever > 100.4 that lasts for 5 days with redness of the lips, tongue, whites of the eyes or peeling around the fingers. This condition is most concerning for its ability to inflame and dilate the coronary arteries of those afflicted. As the CDC and physicians study MIS-C associated with COVID-19, they are looking for similarities as well as differences in these inflammatory responses.
The take away for parents is continued monitoring of your children for signs of any infection. MIS-C is a very rare condition and should not cause parents to be alarmed. However, awareness of this condition can help parents identify concerning symptoms early, which will lead to earlier evaluation and treatment by doctors. Close communication with your pediatrician or primary care provider should start with any of the early symptoms and any acute change in condition would warrant an emergency room evaluation.
As as physician, I have growing concern about the polarity that this virus is causing. It is my greatest hope, that as we all learn more about this virus, we can come together as a vast community to find ways to protect our families, friends and neighbors from this complex virus. Fear of exposure can also lead to missed opportunity to vaccinate and protect children from more common and equally dangerous infections. Sean T. O’Leary, M.D., M.P.H., FAAP, a member of the AAP Committee on Infectious Diseases states, “Parents really shouldn’t be afraid to take their child to their pediatrician if they’re worried they’re sick. They should also, of course, make sure they are keeping up on their well-child care and their vaccinations. The diseases we prevent with vaccines are actually much more severe in children than COVID-19, so we want to make sure to protect children from those diseases.”
Update on Serological Testing (Antibody Testing)
by Dr. Richard Parker
Previously we reported on the utility of COVID-19 antibody testing. Despite the fact that many labs are promoting serologic testing as a way to discover whether individuals have immunity to COVID-19, we recommended against the use of such testing a few weeks ago and at this time nothing has changed with regard to that recommendation. This interesting article shares new information regarding serological (antibody) testing for COVID-19.
There are several methods of antibody testing and some are beginning to appear more accurate than others. The very rapid finger stick type of test called a lateral flow immunoassay (LFIA) appears particularly problematic. Testing using venous blood (generally taken from a big vein in the arm) using a testing method termed ELISA appears to hold more promise for the future.
According to the CDC:
“Serologic testing should not be used to determine immune status in individuals until the presence, durability, and duration of immunity is established.” Stated another way, the science of serologic testing has not advanced enough to offer accurate guidance as to whether someone with antibodies has either short term or long term immunity from COVID-19. The CDC further states: “It cannot be assumed that individuals with truly positive antibody test results are protected from future infection.”
The CDC explains why testing can be wrong so often. A lot has to do with how common the virus is in the population being tested.
“For example, in a population where the prevalence is 5%, a test with 90% sensitivity (meaning the test shows a false negative result 10% of the time) and 95% specificity (meaning the test shows a false positive result 5% of the time) will yield a positive predictive value of 49%. In other words, less than half of those testing positive will truly have antibodies,” the CDC said.
That’s obviously not very helpful. The good news is the predictive value of antibody testing will improve over time…in months, not days or weeks.
So what does SDSM recommend?
Continue all the preventive measures you have heard so much about: social distancing, hand washing and mask wearing. If you become sick, call us immediately and we can help guide you through the process of PCR (nasal swab) testing for the actual virus itself. Once we determine whether you have a COVID-19 infection we will guide you along the path quickly back to health.
While we wait for the science of antibody testing to offer a helpful serologic test we recommend everyone avoid the temptation to jump on antibody testing as it will offer no useful guidance for you, your friends or your medical team. Serological testing is being vigorously studied across the world including the COVID-19 Survivor Study here in San Diego, a collaborative effort between UCSD, Children’s and Scripps Research. Epidemiologic research such as this will eventually answer the immunity question.
Stay tuned!
To Mask or Unmask…that is the question.
by Dr. Richard Parker
In case you have not noticed there is quite a debate occurring across our nation as to the merits of wearing a mask to prevent the spread of COVID-19. President Trump does not seem to like wearing a mask. Former Vice President Biden seems to really like wearing a mask. So the question is to mask or unmask?
You have read in previous emails about how COVID-19 is spread. Essentially transmission occurs from inhaling respiratory droplets laden with the virus from an infected person and by touching an object contaminated with the virus from an infected person then touching your mouth, nose or eyes with your hand (called fomite transmission). Scientific American has a good article on the science of how COVID-19 spreads that offers some guidance to this question. Here is a brief excerpt from the Scientific American Article:
‘According to the U.S. Centers for Disease Control and Prevention and the World Health Organization, the novel coronavirus is primarily spread by droplets from someone who is coughing, sneezing or even talking within a few feet away. But anecdotal reports hint that it could be transmissible through particles suspended in the air. After attending a choir practice in Washington State in early March, dozens of people were diagnosed with or developed symptoms of COVID-19 even though they had not shaken hands or stood close to one another. At least two died. After dining at an air-conditioned restaurant in China in late January, three families at neighboring tables became sickened with the virus—possibly through droplets blown through the air.
To address the prospect of airborne spread of the novel coronavirus, it is first necessary to understand what scientists mean by “airborne.” The term refers to transmission of a pathogen via aerosols—tiny respiratory droplets that can remain suspended in the air (known as droplet nuclei)—as opposed to larger droplets that fall to the ground within a few feet. In reality, though, the distinction between droplets and aerosols is not a clear one. “The separation between what is referred to as ‘airborne spread’ and ‘droplet spread’ is really a spectrum,” especially when talking about relatively small distances, says Joshua Santarpia, an associate professor of pathology and microbiology at the University of Nebraska Medical Center.’
Given this information together with data we shared earlier on air movement within a room vs air movement outdoors, it makes sense to wear a facial covering indoors particularly in smaller rooms, rooms with poor air exchange and certainly when that room is filled with several people. Remember the longer you are in a small room like the one described, the higher the probability of significant airborne viral particle accumulation from an infected person. It generally takes thousands of particles to create an infection. Additionally, the mode of transmission (droplet inhalation into the lungs vs exposure by swiping your nose with a contaminated hand) will dictate how much of the virus would be necessary to create an infection. Inhaling droplets is generally going to deliver the highest number of particles straight into the vulnerable lungs and should be avoided by all means at our disposal. Social distancing is effective at reducing transmission through large particle inhalation, hand washing helps prevent spread from a fomite and the use of a mask reduces the airborne transmission risk described.
With regard to wearing a mask outdoors the data is less clear but common sense would suggest that the accumulation of tiny particles in an outdoor environment with a healthy flow of air would unlikely be significant enough to cause an infection. However, if you are sitting at an outdoor table with several friends within just a few feet of each other laughing and talking loudly, large virus filled particles could easily travel the few feet necessary for you to inhale a large dose of those respiratory particles and end up with an infection despite the fact that air circulation is generally much better outdoors.
Lastly, are certain masks more effective at reducing viral transmission? Absolutely. Cloth masks are generally pretty effective at containing the launch of large particles across a room resulting from a cough or sneeze but they are far less effective at preventing the wearer from inhaling tiny particles while sitting for prolonged periods of time in a small room with lots of people and poor air exchange. Masks worn by medical personnel (N95 or higher) do a much better job at filtering out even the smallest particles the size of a virus and offer better protection to the wearer than cloth masks. These specialized masks are obviously a necessity for those on the front lines of heath care delivery.
So should you mask or unmask?
If you are indoors and with folks other than your “Quaranteam”, wear a mask that covers both your mouth and your nose (remember most of us breathe through our nose). If you are outdoors with good airflow and can socially distance at least 6 feet, a mask is probably less helpful. A cloth mask is fine as long as everyone around you is wearing one. Because by doing so I am protecting you and you are protecting me. It’s the way each of us respects the other.
Bottom line: wear a mask when appropriate, wash your hands frequently (hand sanitizers work well) and socially distance even outdoors. If you follow these simple rules there is a very good chance you will stay healthy.
Wear masks, not gloves in the spread of disease.
Masks and face coverings differ tremendously from gloves in how they prevent disease. Gloves are useful in controlled environments like laboratories and medical procedures, yet in other settings they can increase your exposure to bacteria and viruses. Masks stop the transmission of infective droplets into the environment, while gloves can pick up infective particles and then transfer them to each surface that is touched. The surface of the glove can simply be another host for germs just like your skin. Some gloves have microscopic holes that can be penetrated by germs like viruses and gloves cannot be washed without compromising their integrity. Gloves must be put on and taken off in precise ways to avoid self contamination and hands must still be washed before and after using gloves, even in labs and medical procedures. SDSM recommends the proven method of frequent hand washing, and to avoid the use of gloves. As San Diego begins to re-open and we have more contact with others, it is more important than ever to prevent the spread and a second wave of COVID-19.
Stay safe San Diego.
SDSM continues to be available to help you. Many of you have already enjoyed a telemedicine visit. We can also help you in our thoroughly cleaned and disinfected offices. We disinfect between each patient interaction and ongoing throughout the day. We can safely see you in person for general physicals, annual health assessments, management of chronic conditions, and treatment of injuries. Cold/flu/COVID-19 symptoms and patients at increased risk of complications from COVID-19 are best addressed through a convenient telemedicine appointment, as are on-going treatment assessments and check-ins with your provider.
Remember if you have diabetes, asthma, COPD, heart problems, impaired immune function, difficulty getting enough sleep, or are experiencing high levels of stress, it is important to call us. Working together, we can keep you healthy and safe.
Yours in health,
The Physicians and Staff of San Diego Sports Medicine and Family Health Center
